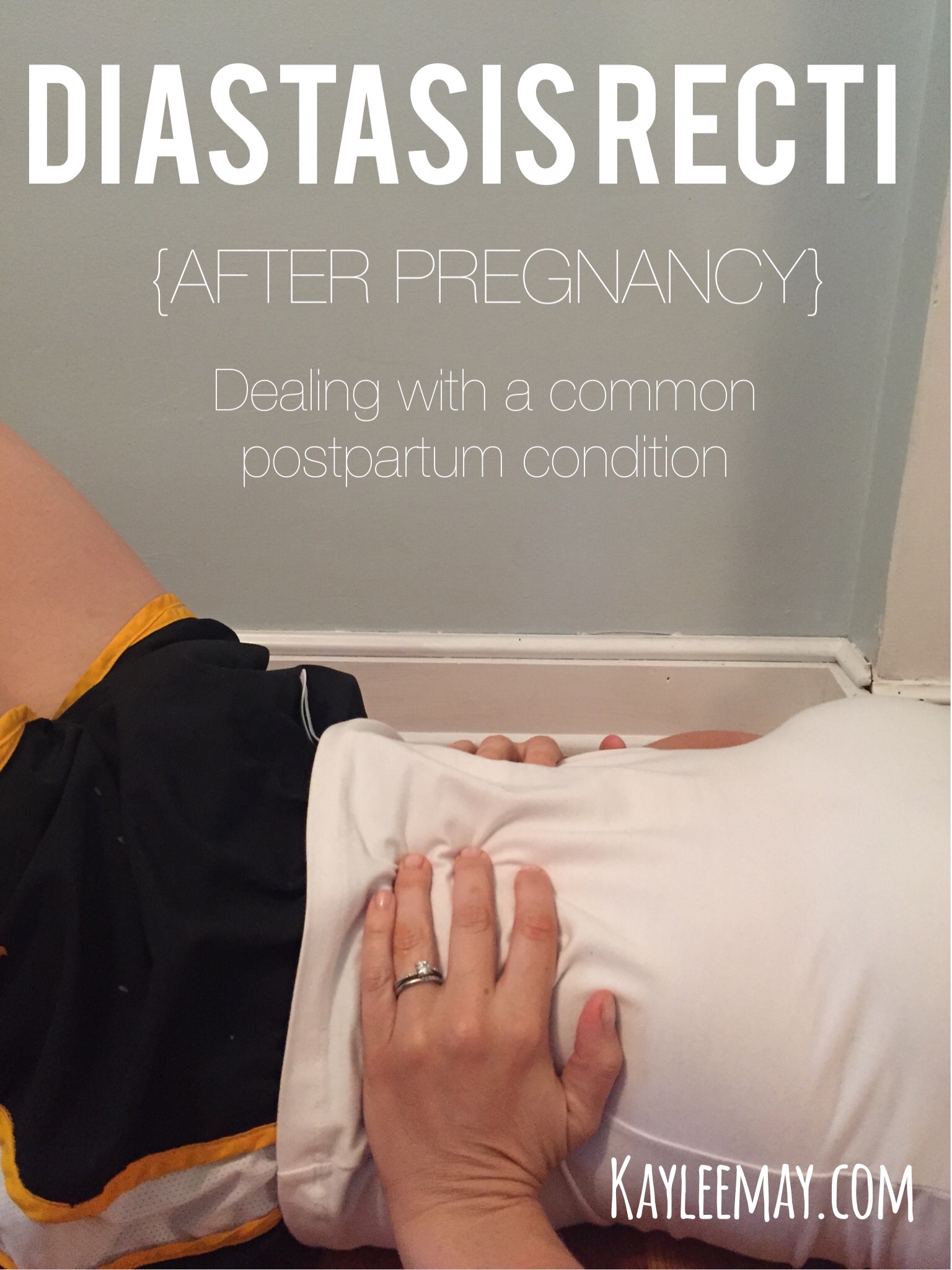
My labor and delivery nurse has encouraged me to write about and share my birthing experience with Rosalie since it was so calm and actually, quite nice. She mentioned that women often come into the hospital hoping for a natural birth, but haven’t prepared for it. So here is a little background on my previous birthing experience, information about how I prepared for my second birthing experience, and Rosalie’s birth story….which is long and boring (fortunately for me). I wrote this in random times between my girls’ naps, in the middle of the night, etc, so excuse the length and grammatical errors.
Seton’s birth (my first), while wonderful and miraculous, was somewhat of a doozy. I went into labor with the plan of getting an epidural and hopefully coasting through delivery. I knew that labor/delivery rarely went exactly according to plan, so I was fairly open to the idea that things might change. I was very fortunate that I progressed well and she was able to be born safely, but the epidural didn’t work. Well, it worked for about two glorious hours, then for some reason just stopped. The nurses had me turning on my sides, changing how much the bed was reclined, and even called in the anesthesiologist to alter the placement and dosage (when I was at 9 cm). It was miserable feeling stuck in the bed through transition. I remember telling them to let me sit up better in bed because I was going to push whether they liked it or not–the urge to push was so strong. I was wishing I didn’t even get the epidural because then at least they would let me get out of bed.
I decided I would prepare for a natural, unmedicated birth for my second child, and if I were to need an epidural I would get one. I knew that this time around, I needed a strategy for dealing with contractions. I kept thinking that birthing is the most natural and common thing in the world–every person in the world has experienced it–it shouldn’t be so traumatic.
Like I said, I want to emphasize the importance of preparation. Here are some key ways I prepared for birth:
1). Home study course with Hypnobabies.
2). Listening to the recommended tracks daily.
3). Eating healthy (eh, I should say MOSTLY eating healthy) and exercising.
4). Listening to Fear Free Childbirth podcast on my way to/from work. I LOVED hearing women’s birthing stories that WEREN’T all about pain, trauma, and drama.
5). This sounds SUPER weird of me, but I think it REALLY helped….watching youtube videos of hypnobirths. You know how athletes do mental imagery before big games/meets? Seeing calm births helped me envision myself having one. The only other births I’ve ever “witnessed” were from movies, and we all know those are completely unrealistic. But that’s what we imagine going into labor….so wrong!
My sister-in-law told me about hypnobirthing and sent me her home study guide. I read Marie Mongon’s book as well as Ina May Gaskin’s Guide to Childbirth. The more I read about healthy, natural, calm birthing experiences, I knew that it was possible for me as well. One thing I love about hypnobirthing is the emphasis on staying relaxed. With my background in physical therapy, I completely understand how tensing up can increase your pain and put you at greater risk for birth injuries.
I started around week 28 of my pregnancy going through the home study guide and listening to the recommended hypnosis tracks every day. I remember thinking at the beginning of the home study that there was no way I could be hypnotized. I was envisioning Davey having to dangle a watch in front of my eyes and tell me I was getting veeeery sleepy…., but that’s not how it works. It’s more like being hypnotized in the same way as when you are watching TV or reading an article on your phone and you somehow completely drown out your spouse (sorry, Davey). I was able to drown out everything while I was having pressure waves (pressure waves is the hypnobirthing term for contractions). My focus was entirely on staying relaxed. This took a lot of practice leading up to the birth. I think I was able to easily go into my relaxed state during Rosalie’s birth because I had practiced it so much (every day).

Okay, onto the boring birth story!
I woke up on Sunday, September 11 (6 days after the due date my doctor gave me but EXACTLY on the due date I gave myself based on Fertility Awareness Method/NFP I have to add-ha!) at 2am with some pressure under my belly. This was very different than the crampy contractions I had with Seton, so I wasn’t sure it was “it.” But they started coming every 7-8 minutes and were pretty intense, so I decided to put on a hypnobirthing track with my headphones. At some point between 2am and 7am I went to the bathroom and Davey woke up saying, “is this it?” I was pretty dumb and said, “Yes! They’re 7-8 minutes apart, so maybe the baby will be here by noon!” HA! I laugh at that so much now–
Seton woke up at 7am and contractions slowed to 30 minutes apart (or more) throughout the day. It was a fairly relaxing day–I watched ‘The Intern’ with my mom and sat on the porch as Seton played with Davey in the corner. Every time a pressure wave came on, I closed my eyes and breathed in for a count of 4 and out for a count of 8 and focused on staying relaxed. I was a little anxious and upset that contractions had slowed down and that extra time allowed some fear to creep back in–what if it’s too painful? What if it’s as bad as last time? I debated going for a walk to “speed things up,” but then wondered why there is always a push to “speed things up” with birthing? What’s the rush? The pressure waves were tolerable. I was home. I was eating and moving and feeling well. The baby was healthy–I felt her kicking. I decided it was best to relax since I knew I would need energy later. At some point I laid back down in my room and listened to a Fear Release track that was intended to help me let go of any fear I have with birthing–I think I fell asleep and had a nice nap. 🙂 I also remember deciding wash and straighten my hair since I knew I wouldn’t be able to for a few days (priorities, ladies).
We went to bed around 10 that night and pressure waves started up again around 11pm. I started timing them–and again they were 7-8 minutes apart. I wanted to focus on staying relaxed, so I woke Davey up to time them. I regret this–at the time, I thought things would REALLY pick up quick and we would be leaving for the hospital soon. They were 7-8 minutes apart ALL NIGHT and poor Davey didn’t sleep a wink. I was able to sleep between pressure waves as I was listening to relaxing tracks. I kept waiting until the “under 5 minutes for an hour” rule to head to the hospital. I was afraid they would just slow down again during the day, and I didn’t want to be at the hospital for that. 7am rolled around again, and Seton was calling to us to get her out of her crib. I couldn’t believe I was still home!
We sent her to daycare–(I gave her one last hug as my one and only and was a little emotional knowing her life was about to change so much)– and by that point I was a little frustrated, tired, and slap happy. We don’t have a birthing ball, so I was jokingly bouncing on one of Seton’s blow up horses, and my mom and I had some good laughs. I decided to take a bath, then try to sleep a little. I laid in my room by myself, listened to some tracks, and fell asleep. Every time I felt a pressure wave, I hit the “lap” button on my iPhone’s stopwatch, barely opening my eyes. I laid like that for almost two hours. When I decided I should use the bathroom, I looked at the timer and saw that I had been having contractions just 3-4 minutes apart for 2 hours. I couldn’t believe it! I had been so relaxed, it felt like I was sleeping between pressure waves that were 20 minutes apart.
I told Davey about the timing and asked him to make me lunch (love him) while I called my doc and told her I was headed to the hospital.
As we were walking out the door, I felt fear creep back in a bit. I hugged my mom (who was staying with us to take care of Seton) and held back a few tears–hugging my mom before giving birth was really emotional because I knew she had gone through all this FOR ME before. I felt very appreciative of her and truly felt life coming full circle. 🙂
I got in the car and said to Davey, “I can’t believe Mary rode a DONKEY through this!” The pressure waves were definitely more intense, and I was nervous about going through transition on the way to the hospital. I turned on my Birthing Day hypnobirthing track and put my ear buds in and kept my eyes closed the whole way. (this was MUCH different from driving to the hospital with Seton when I was yelping in pain). We were at the hospital so fast—time seemed to be nonexistent that day. I think we arrived shortly after 12:00.
Davey quickly told the nursing staff that I was doing hypnobirthing, and I did NOT want to know how dilated I was. I didn’t want to be told I was 3 cm after laboring for a day and a half–I would have felt so defeated. I also didn’t want to know if I was really close because I didn’t want to become fearful or anxious. I just wanted to BE. From everything I have read about dilation, it doesn’t really matter. It doesn’t predict how close or how far you are from birthing your baby. Things can “speed up” or “slow down.” So I just wanted things to go as they should.
A few weeks before Rosalie’s birth, my doctor informed me the nurses at the hospital were on strike. I LOVED my nurses with Seton, so I panicked a bit and wondered if the replacement nurses would be as skilled. Davey and I decided to pray every night for our labor/delivery nurse. After I was checked and determined to be in true labor, a very sweet nurse came in and introduced herself–LeShanta. Davey again told her we were doing hypnobirthing, and she responded by telling us she is also a certified doula and has been present for many other hypnobirths. I literally got goosebumps—we had been praying for her. God was present, and I KNEW that everything would be ok. It was like God was saying, “I have planned this out for you. Just let go.”
Walking out of the triage room, I felt a strong pressure wave. I stopped to do my breathing, and LeShanta whispered in my ear, “spread your feet apart” as she put her hand on my shoulder–a hypnobirthing cue to relax and release. Such small things, but the gentle reminders helped me so much.
When we got the to labor/delivery room, I just wanted to lay on my side and listen to my tracks. I did. I kept my eyes closed. Davey would occasionally give me sips of water or Gatorade and remind me to get up and pee. I wanted him to keep his hand on my low back during pressure waves…for some reason it felt like some of the energy went to him, which was wonderful. I remember one pressure wave was so intense that I clenched my fists. LeShanta gently opened my fingers which was enough of a reminder to me to relax.
The doctor came in around 3:00 (I think? I just remember her saying, “I’ll be back at 3:00” after I initially got to the room). She asked me to lay on my back (my thoughts: NO! PLEASE NO!). I did. She checked my dilation and just as she was checking, the strongest and by far the most painful pressure wave came on. I said, “OUCH! THIS IS THE WORST YET! OUCH!” and I heard LeShanta whisper, “Release” with her hand on my shoulder which immediately relaxed me and brought me back to my breathing. It was like the contraction was instantly not painful anymore–just pressure. That’s when I realized my hypnobirthing was VERY SERIOUSLY WORKING if I just stay in the zone. I had gotten out of the zone when the doctor was checking me.
The doctor left the room after telling me, “don’t push yet. We aren’t ready.” I laid back on my side. LeShanta told me I should put my earbuds back in because she was going to be getting the room ready and didn’t want me to get distracted. A few contractions later, I felt my body push Rosalie down. I told LeShanta, and she whispered, “that’s okay. It’s doing what it’s supposed to.”
When the doctor came back in, I had a couple gentle pressure waves, then another where my body pushed Rosalie down (very neat feeling!). The doctor immediately yelled “she’s delivering!” and had me lay on my back. Being on my back was a little miserable and not my first choice. I do wish I had told the doctor to let me birth on my side. It was so much more comfortable. I got out of my “zone” when trying to get in the right position, but LeShanta calmly whispered things in my ears that helped me get back and birth my baby easily. (voice of an angel!) The doctor mentioned the baby was being born in the water bag and she was breaking it as Rosalie was on her way out.
A few minutes later at 3:35pm and Rosalie was in my arms.

It turns out I was 7cm when I got to the hospital and 9cm when my doctor checked me around 3pm (and when I had that intense contraction). The whole time I was at the hospital I was anticipating the dreaded “transition” that everyone talks about. I didn’t realize until my body started pushing Rosalie out that I had already passed transition. I never once had the thought of “I can’t do this anymore” which is apparently the classic sign of transition. THANK YOU, HYPNOBIRTHING.
I felt so good after her birth. It felt so normal and natural; I loved that I wasn’t hooked up to monitors and could get up whenever I needed to use the bathroom. I had been snacking and eating, and laying on my side the whole time so I wasn’t completely drained. LeShanta was so calm. She kept the lights dim, spoke in soft tones, and never showed and sense of hurry. It was great.
I told LeShanta a few days ago that Rosalie is such a calm baby, and speaking of research, she said: “Mothers who have natural, relaxed labors, and who have practiced relaxation throughout pregnancy have more peaceful and laid-back babies.” I have SOOOOO witnessed that with Rosalie. Aside from a little fussiness since her 2 month shots, she has been such an easy baby. She’s very calm and happy.


I highly recommend preparing for labor with hypnobirthing, even if you’re 100% set on pain meds or if you need a C-section. It will help so much to get you through pressure waves and to have a relaxing pregnancy.
Being a woman is the greatest–we have both the physical strength to grow a human within us and bring that human into the world as well as the emotional strength to selflessly give our bodies so that someone else can have life.
Giving birth to my children is my greatest accomplishment and my greatest joy.
Now onto raising them…